Health and Human Services Secretary Robert F. Kennedy Jr. forced major shifts in federal policy over the last year toward his personal anti-vaccine views, dismantling an immunization advisory panel and filling it with allies. Now physicians, medical groups, and lawmakers fear he may run the same playbook on another federal guidance body, compromising recommendations that primary care doctors rely on and that inform no-cost insurance coverage requirements for tens of millions of Americans.
In a series of congressional hearings earlier this month, Kennedy criticized the U.S. Preventive Services Task Force (USPSTF) and announced plans to add new members. The independent panel provides guidance on a wide range of routine preventive care, not including vaccines, that primary care doctors provide to children and adults.
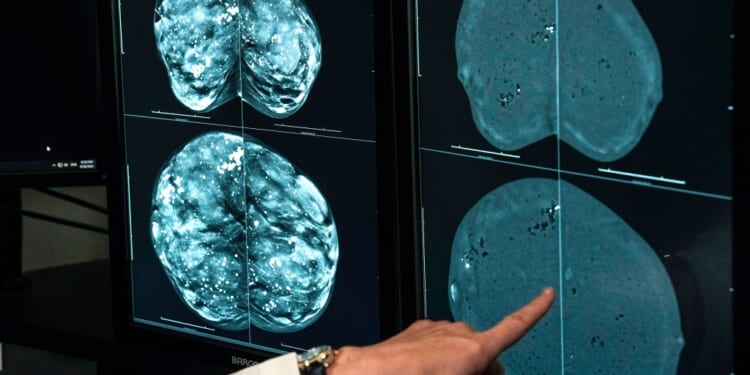
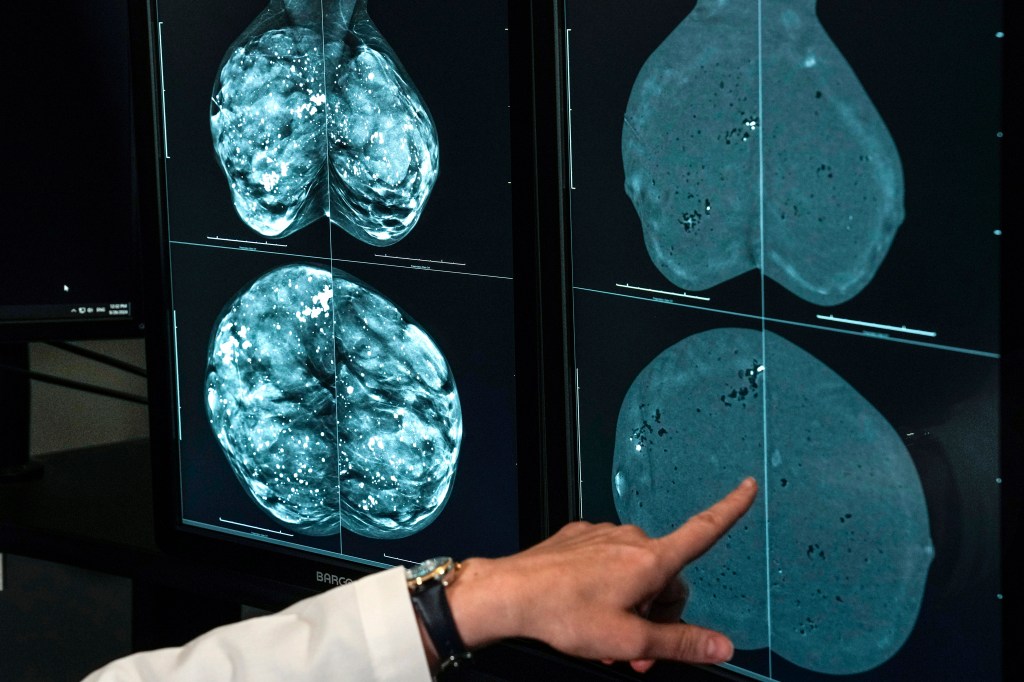
The task force, made up of 16 volunteers, maintains nearly 100 care recommendations—from breast cancer screening to statin prescriptions for people at risk of cardiovascular disease to depression screening. The guidance involves only preventive services the task force assesses are effective interventions for otherwise healthy people mostly provided or recommended by primary care doctors during routine visits. This prevention care is distinct from treatment for people who are exhibiting signs or symptoms of a particular illness.
“Anytime anyone goes to their doctor for a wellness exam, anytime their doctor says, ‘Oh, you should do this to stay healthy,’ it’s usually based on the U.S. Preventive Services Task Force recommendations,” Dr. Alex Krist, former chair of the USPSTF who served on the body from 2014 through 2021, told The Dispatch. “Every primary care clinician uses the task force recommendations 100 times a day.”
HHS established the first iteration of the task force during the Reagan administration in 1984, and it gradually became more formalized and structured over the ensuing decades as researchers and doctors developed systems for critically evaluating the effectiveness of clinical care. The Affordable Care Act elevated the significance of the task force by requiring health insurance to cover at no cost to patients the preventive services to which the task force gives an A or B rating.
“The USPSTF introduced rules of evidence, systematic search methods to ensure a comprehensive review of all relevant studies, a scoring system for rating studies, and letter grades to link recommendations to the quality of the science,” Drs. Robert Lawrence and Steven Woolf, the task force’s first chair and the first scientific adviser, respectively, wrote earlier this year.
The task force is composed of volunteers from outside of the government and is supposed to be scientifically independent, but the HHS secretary has direct involvement in selecting the panel’s 16 members, who each serve four-year terms. The Supreme Court ruled last year that the secretary has the authority to remove members at will and can unilaterally reject or revoke any of the task force’s recommendations. Lawrence and Woolf, along with a chorus of other former task force members, fear that the Trump administration could compromise that careful system of evidence evaluation.
‘Lackadaisical and negligent.’
Kennedy has effectively put the task force on ice for the last year. The Wall Street Journal reported last July that Kennedy intended to fire all 16 members. But the administration opted to keep the body dormant, canceling its July and November meetings as the secretary focused on vaccine issues throughout the fall. In December, the terms of five of the 16 members expired without any announced plans for replacements, and Kennedy also canceled the March task force meeting. The USPSTF has now missed a full year of meetings; more than a dozen draft recommendations, including guidance on medication to reduce breast cancer risk, autism screenings, and smoking interventions, are stuck in the pipeline.
Earlier this month, Kennedy levied broad criticisms against the task force, similar to the castigations that presaged his reconstitution of the Centers for Disease Control and Prevention’s vaccine panel. “We are reforming now the USPSTF,” Kennedy told the House Ways and Means Committee. “That committee has been lackadaisical and negligent for 20 years. We are bringing on new members who have a clear mission. We’re going to have much more frequent meetings. We’re going to have, for the first time, transparency.”
Last week, the administration published an application call for new members that included a widened range of backgrounds and qualifications. Previously, the task force strongly favored new members who were practicing primary care doctors with training in evidence evaluation and research analysis. The recent notice explicitly encouraged nominations of physicians with backgrounds in care specialties beyond primary care, as well as individuals with experience in developing healthcare recommendations on behalf of employers, health systems, and policymakers in Congress. Kennedy told the Senate Finance Committee that medical specialties have not been sufficiently represented by the task force.
Primary care vs. specialists.
The secretary’s critique of the task force involves a long-standing debate about its structure: Who is best positioned to evaluate decisions on preventive care guidelines? Is it the primary care doctors who deliver and refer people for preventive services, or physicians who specialize in the specific conditions the services are designed to detect and prevent?
“This debate’s been going on for 40 years since the task force was founded,” said Dr. Barron Lerner, an internist at New York University’s medical school and a historian whose research has examined the history and evolution of the USPSTF. “The folks doing evidence-based medicine were of a very strong opinion that the best way to avoid biasing [recommendations] was to use generalists who have no skin in the game.”
Former task force members insist that maintaining the primary care membership is crucial to the credibility and effectiveness of recommendations. “Specialists are specialists at diagnosing and treating diseases, and that’s a different thing than prevention,” Krist said.
He argued that the comparatively narrow frame of a specialist can result in supporting screening and care that would be the right call for an individual exhibiting symptoms of disease but would not be a net benefit as a population-level recommendation for healthy people. “A specialist who’s treating someone who has a chronic disease, by definition, they have signs and symptoms, and they’re experiencing harms from their chronic disease,” Krist added. “What that means is that we’re willing to accept a little bit more harms from the tests and procedures and medicines that we give to someone because they’re already experiencing harms from their disease, but with prevention, there’s a different bar.”
Dr. Michael Barry, who served on the task force from 2017 to 2024, including as vice chair and chair, told The Dispatch that prioritizing specialty membership would be challenging since the USPSTF makes recommendations on so many different areas of care. For example, what expertise would a radiologist bring to bear on depression screening guidance?
Specialty doctors have pushed back against the primary care preference, arguing that more granular expertise and exposure to the consequences of illnesses often detected too late should inform the guidance. Fierce debates have raged over task force recommendations, particularly regarding what age universal breast cancer screening should begin and at what frequency. Lerner, who wrote an entire book about the so-called breast cancer wars, said that this disagreement drove the task force to get better at including and consulting the relevant specialists throughout the process of researching and drafting new and updated guidelines, but its membership has remained dominated by primary care doctors and methodologists.
Trust and trade-offs.
Barry and Krist both emphasized that the ultimate effectiveness of the recommendations depends on the trust that primary care physicians place in the task force. Specialty medical organizations have long made their own recommendations, and part of the original purpose behind the task force was helping doctors sift through a river of specialist guidance to figure out what’s the best preventive care for their patients. If the task force is remade as a specialty representation body, they argue, it could reduce primary care trust in the recommendations.
“Primary care doctors are bombarded with information from all angles,” Barry said. “How does a primary care doctor sort all the recommendations from different specialty societies in making recommendations for their patients?”
Kennedy has signaled that he already has specific recommendations in his sights, telling the House Energy and Commerce Committee that “if [USPSTF] had been doing its job, we would have early screening for Alzheimer’s.” The task force has previously concluded that the evidence for measurable benefits from early screening was insufficient to make a recommendation but had drafted a research plan last year to revisit the issue before Kennedy canceled the meetings.
The USPSTF has changed its mind in the past on recommendations, but researchers and members emphasize that it plays a crucial role in evaluating the trade-offs involved in any preventive intervention and refusing to endorse practices in the absence of strong evidence of improved health outcomes.
“The task force’s greatest accomplishment is its efforts—not always successful—to convey the fact that more screening is not always better,” Lerner said. He argued that specialist societies and physicians tend to err toward more testing. “You’d be hard pressed to find [gastrointestinal] doctors or radiologists arguing that the task force is too liberal. They’re always arguing the task force is too conservative.”
Concern from lawmakers.
Major medical groups, as well as some key lawmakers, fear an iconoclast like Kennedy is the exact opposite kind of person suited to improve the task force, particularly in light of his broad-brush indictment of 20 years of USPSTF’s work and his track record with the vaccine committee. Nineteen Democratic senators sent Kennedy a letter last month criticizing him for canceling the task force meetings and worrying he might appoint unqualified new members. Sen. John Barrasso, a Utah Republican and one of the chamber’s few physicians, also expressed worries about how constructive Kennedy’s planned changes would be.
“As a doctor, I’ve relied on these recommendations over the years. They’ve helped shape the standard of care across the country from cancer screening to heart health,” Barrasso said during a hearing with Kennedy earlier this month. “The task force’s methodology is grounded in an independent review of the evidence, careful evaluation of the benefits and the harms.”
Kennedy told the senator that he wouldn’t undermine the task force’s function as the gold standard for primary care doctors and that he only wanted “a more representative group of specialties.” Barrasso pressed him on changes, not in the task force’s membership, but in how USPSTF evaluates and assesses scientific evidence. “So you believe the current methodology, the way they do it, is still the gold standard?” Barrasso asked.
“I think there are some limitations we are trying to address,” Kennedy replied.